
A toothache that wakes you up at 2 a.m. or makes it impossible to concentrate at work is your body sending an unmistakable signal: something is wrong inside the tooth. The pulp — the soft tissue containing nerves, blood vessels, and connective tissue deep within each tooth — can become infected or inflamed from deep decay, cracks, or trauma. When that happens, a root canal is often the only way to save the tooth and eliminate the pain.
The challenge is that pulp damage does not always announce itself with dramatic pain right away. Some warning signs are subtle, and patients on Long Island frequently tell us they ignored early symptoms for weeks or months before the situation became urgent. Knowing what to watch for can mean the difference between a straightforward root canal and an emergency extraction. Below are the five signs our dentists at Meadowbrook Dental Care see most often, along with what causes root canal infections, what the procedure actually involves, and what happens if you delay treatment.
1. Persistent, Throbbing Toothache That Won't Go Away
A toothache that lingers for days rather than hours is the most common reason patients seek emergency dental care. The pain may be constant or come in waves, but it does not resolve with over-the-counter painkillers the way a minor sensitivity issue would. You might feel a deep, throbbing ache that radiates into your jaw, ear, or temple on the same side of your face.
This type of pain typically indicates that the nerve inside the tooth is inflamed or dying. As bacteria multiply within the pulp chamber, they produce gases and toxins that increase pressure inside the tooth — a rigid structure with no room to expand. That pressure on the nerve is what creates the relentless, throbbing quality that distinguishes a pulp problem from ordinary tooth sensitivity. If the pain is severe enough to disrupt sleep or daily activities, do not wait for your next scheduled cleaning. Call for an evaluation as soon as possible.
2. Prolonged Sensitivity to Hot and Cold
Momentary sensitivity when you sip hot coffee or bite into ice cream is common and usually harmless — it often points to mild enamel erosion or gum recession. The red flag is sensitivity that lingers for 30 seconds or more after the hot or cold stimulus is removed. If you take a drink of ice water and the sharp, aching sensation persists long after you swallow, the pulp inside the tooth is likely compromised.
Lingering sensitivity occurs because inflamed or damaged nerve tissue overreacts to temperature changes and cannot calm down the way healthy pulp does. Over time, the sensitivity may intensify or shift from cold triggers to heat triggers — a progression that often signals the nerve is transitioning from reversible inflammation (pulpitis) to irreversible damage that only a root canal can address.
3. Darkening or Discoloration of a Specific Tooth
If a single tooth turns noticeably gray, dark yellow, or brown compared to its neighbors, the internal tissue may be breaking down. This discoloration happens when the blood supply to the pulp is disrupted — often from trauma such as a blow to the face, a sports injury, or even a fall that happened years earlier. The tooth may not have hurt at the time of the injury, so patients are sometimes surprised when the color change appears months or years later.
Internal discoloration is different from surface staining caused by coffee, tea, or tobacco. Surface stains affect multiple teeth and can be addressed with professional whitening. A single darkened tooth, however, suggests that the nerve is dead or dying and that bacteria may already be colonizing the empty pulp chamber. A root canal removes the necrotic tissue, stops the infection, and preserves the tooth structure so it can be restored with a dental crown that matches the color of your surrounding teeth.
4. Swollen or Tender Gums Near the Affected Tooth
Gum tissue that is swollen, red, or tender in a localized area — right next to one specific tooth — can indicate that infection has spread beyond the tooth's root tip and into the surrounding bone and soft tissue. In some cases, a small pimple-like bump called a fistula or parulis forms on the gum. This bump is actually a drainage channel for pus, and pressing on it may produce a foul taste in your mouth.
A dental abscess is a serious condition. Left untreated, the infection can destroy the jawbone around the tooth, spread to adjacent teeth, or — in rare but dangerous cases — enter the bloodstream and affect other parts of the body. If you notice localized gum swelling accompanied by facial swelling, fever, or difficulty swallowing, seek emergency dental treatment immediately. This is not a situation that can wait until Monday.
5. Pain When Biting, Chewing, or Touching the Tooth
Healthy teeth should not hurt when you bite down on food or tap on them with a fingernail. If applying pressure to a specific tooth produces a sharp jolt of pain, the ligament surrounding the root may be inflamed due to infection spreading from the pulp. Dentists test for this during an exam using a technique called percussion — gently tapping each tooth with an instrument to isolate which one reproduces the pain.
Bite sensitivity can also result from a cracked tooth, which is one of the common causes of pulp infection in the first place. Cracks allow bacteria to bypass the protective enamel layer and reach the pulp directly. If the pain is consistent and worsening, a root canal combined with a crown is often the best path to saving the tooth and restoring full function.
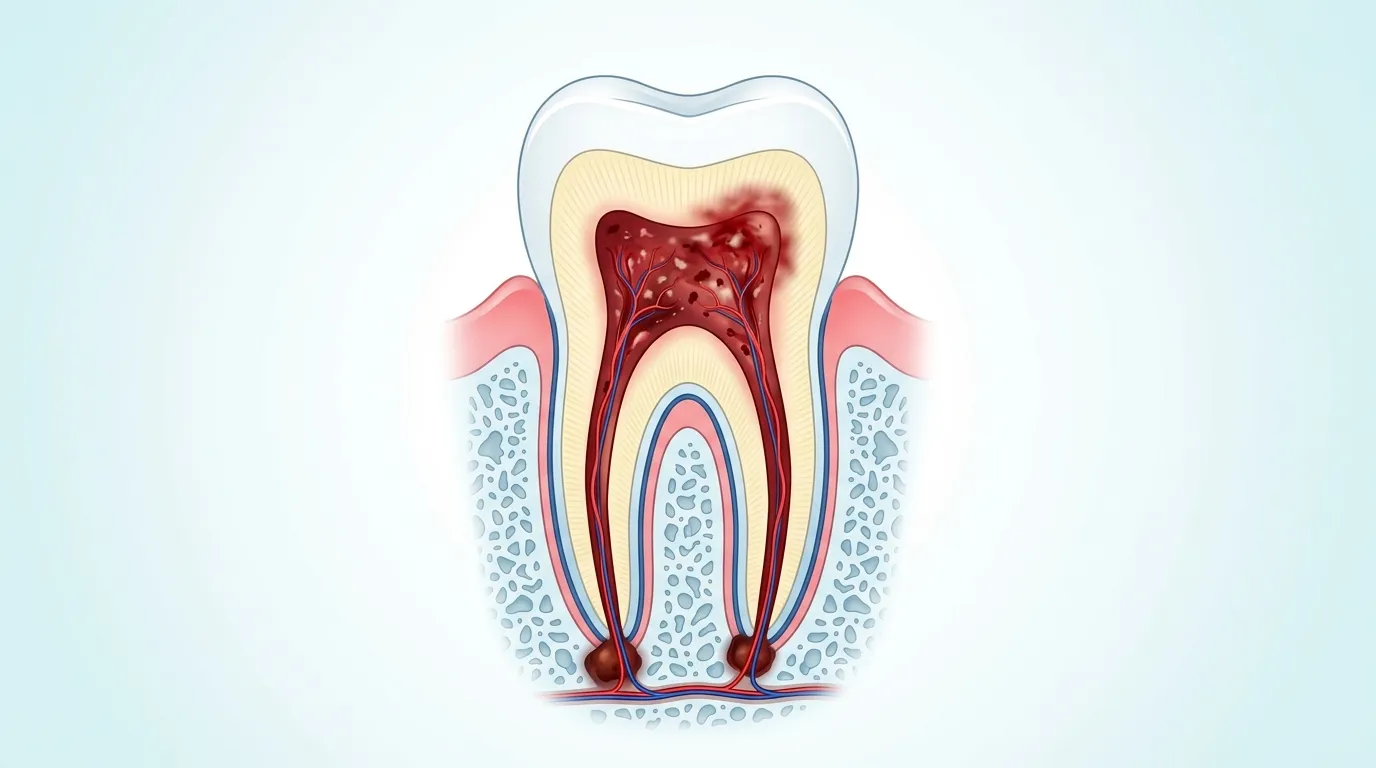
What Causes Root Canal Infections?
Understanding the cause helps you understand why the treatment is necessary. The most common reasons the pulp becomes infected or irreversibly inflamed include:
- Deep, untreated cavities — Tooth decay that penetrates through enamel and dentin eventually reaches the pulp chamber, allowing bacteria direct access to the nerve.
- Cracked or fractured teeth — Even hairline cracks can act as highways for bacteria. Cracks often result from biting on hard objects, grinding (bruxism), or trauma.
- Repeated dental procedures — A tooth that has had multiple fillings or other restorations is at higher risk because each procedure removes a bit more protective tooth structure and brings instruments closer to the pulp.
- Trauma — A blow to the mouth can sever the tooth's blood supply even if there is no visible crack. The pulp slowly dies over time, and infection follows.
What Actually Happens During a Root Canal
The phrase "root canal" carries a reputation that modern dentistry no longer deserves. Decades ago, the procedure was genuinely uncomfortable. Today, with advanced anesthesia, rotary instruments, and the option of sedation dentistry, a root canal is comparable to getting a large filling. Most patients at our Nassau County offices report feeling pressure but no pain during the procedure.
Here is what the process looks like step by step. Your dentist administers local anesthesia to completely numb the area. A small opening is made in the top of the tooth to access the pulp chamber. Using specialized instruments, the infected or inflamed pulp tissue is removed from the chamber and the root canals. The canals are cleaned, shaped, and disinfected. A biocompatible rubber-like material called gutta-percha fills the empty canals, and the opening is sealed with a temporary or permanent filling. In most cases, a dental crown is placed over the tooth within a few weeks to restore full strength and protect against fracture.
The entire appointment typically takes 60 to 90 minutes for a front tooth and up to two hours for a molar with multiple roots. Most patients return to work or normal activities the next day.
Root Canal Cost on Long Island
Cost is one of the first questions patients in Mineola and Plainview ask, and the answer depends primarily on which tooth needs treatment. Front teeth (incisors and canines) have a single root canal, making the procedure faster and less expensive. Premolars have one or two canals, and molars typically have three or four, which increases the complexity and time required.
- Front tooth root canal: $800–$1,000
- Premolar root canal: $900–$1,200
- Molar root canal: $1,000–$1,500
These figures do not include the crown that is usually placed afterward ($1,000–$1,800), but they represent the root canal procedure itself. Most dental insurance plans classify root canals under "major services" and cover 50–80% of the fee after your deductible. Our team will verify your benefits before treatment so you know exactly what to expect out of pocket.
Disclaimer: These cost ranges are educational estimates for the Long Island area. Your actual cost depends on tooth location, number of canals, and your insurance plan. A personalized quote requires an in-office evaluation.
Symptoms Comparison: Root Canal vs. Normal Sensitivity vs. Cracked Tooth
| Factor | Root Canal Needed | Normal Sensitivity | Cracked Tooth |
|---|---|---|---|
| Pain type | Persistent, throbbing, deep | Brief, sharp, fleeting | Sharp pain on biting, may release on opening |
| Duration | Lingers 30+ seconds, may last hours | Fades within seconds | Intermittent, triggered by specific biting angles |
| Temperature response | Severe lingering pain to hot or cold | Mild reaction that resolves quickly | Cold sensitivity common, may not linger |
| Gum swelling | Possible, localized near one tooth | None | Rare unless crack extends below gum line |
| Tooth discoloration | Possible darkening | None | None unless nerve damage occurs |
| Urgency | High — see dentist within days | Low — mention at next cleaning | Moderate to high — prompt evaluation recommended |
| Typical treatment | Root canal + crown | Desensitizing toothpaste, fluoride | Crown, root canal if crack reaches pulp |
What Happens If You Don't Get the Root Canal
Delaying or avoiding a root canal does not make the problem go away — it makes it worse. The infection inside the tooth will continue to spread. A dental abscess can form at the root tip, destroying surrounding bone and creating a pocket of pus that causes significant facial swelling and pain. In some cases, the infection erodes enough bone that the tooth becomes loose and must be extracted entirely.
Beyond the tooth itself, untreated dental infections carry systemic risks. Bacteria from an abscessed tooth can enter the bloodstream and contribute to complications elsewhere in the body. In extreme cases, infection can spread to the neck, creating a life-threatening condition called Ludwig's angina, or reach the brain and cause a brain abscess. These outcomes are rare but entirely preventable with timely treatment.
There is also a financial cost to waiting. A root canal and crown today may run $2,000–$3,000 total, but an extraction followed by a dental implant to replace the missing tooth costs $3,000–$5,500. Saving your natural tooth is almost always the better clinical and financial choice when it is still an option.
Frequently Asked Questions
Is a root canal painful?
Modern root canals are performed under local anesthesia, and most patients compare the experience to having a filling placed. You may feel pressure but should not feel pain. Meadowbrook Dental Care also offers sedation options for patients with dental anxiety, so you can be completely relaxed throughout the procedure.
How long does recovery take after a root canal?
Most patients experience mild soreness for two to three days after the procedure, manageable with over-the-counter anti-inflammatory medication like ibuprofen. You can typically return to work the day after treatment. The tooth may feel slightly different from your other teeth for a few weeks as the surrounding ligament heals, but significant pain after a root canal is uncommon.
Can a tooth that needs a root canal heal on its own?
No. Once the pulp inside a tooth is infected or has died, the body cannot repair it. Antibiotics can temporarily reduce swelling and manage the infection, but they cannot eliminate bacteria inside the sealed canal system. Without a root canal, the infection will return — often worse than before.
Do I always need a crown after a root canal?
In most cases, yes. A root canal removes the internal tissue that supplied moisture and nutrients to the tooth, making it more brittle over time. A crown encases the tooth and distributes biting forces evenly, preventing fracture. Front teeth occasionally receive a filling rather than a crown, but molars and premolars almost always need full crown coverage to function safely long-term.
If any of these warning signs sound familiar, do not wait for the problem to escalate. Call Meadowbrook Dental Care at (516) 284-1234 (Mineola) or (516) 346-5757 (Plainview), or schedule online to book a diagnostic exam and get the answers you need.
Don't Wait Until the Pain Gets Worse
If you're experiencing any of these warning signs, a quick exam at our Mineola or Plainview office can determine exactly what's going on — and get you out of pain fast.